
My Blog
-
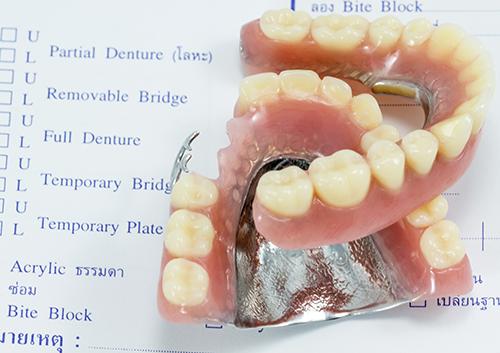
Care for Your Dentures
updated: Apr. 30, 2024

-
Infant Teething Remedies: What Might Help—And What to Avoid
updated: Apr. 23, 2024

-
Every Day is Earth Day
updated: Apr. 16, 2024

-
How Sedation Dentistry Can Help You Overcome Dental Anxiety
updated: Apr. 09, 2024

-
Do Spring Allergies Mean (B)Looming Dental Problems?
updated: Apr. 02, 2024

-
Avoid the Emergency Room for Dental Problems
updated: Mar. 26, 2024

-
Steer clear of that candy!
updated: Mar. 19, 2024

-
Going Green for St. Patrick’s Day?
updated: Mar. 12, 2024

-
March is National Nutrition Month!
updated: Mar. 05, 2024

-
What did the first dentures look like?
updated: Feb. 27, 2024
-
Let's Talk About Your Roots!
updated: Feb. 20, 2024

-
Team Dark Chocolate
updated: Feb. 13, 2024

-
Keeping Your Teeth Strong and Healthy
updated: Feb. 06, 2024

-
When snoring becomes more than just annoying: The dangers of sleep apnea
updated: Jan. 30, 2024

-
Ten Fun Things to Do with Your Old Toothbrush
updated: Jan. 23, 2024

-
Top Reasons People Choose Veneers
updated: Jan. 16, 2024

Our Locations
Find us on the map
Hours of Operation
Our Regular Schedule
Long Island City
Monday:
9:00 am-6:30 pm
Tuesday:
9:00 am-5:00 pm
Wednesday:
9:00 am-6:30 pm
Thursday:
9:00 am-5:30 pm
Friday:
Closed
Saturday:
9:00 am-2:00 pm
Sunday:
Closed
Manhattan
Monday:
Closed
Tuesday:
Closed
Wednesday:
Closed
Thursday:
9:00 am-5:00 pm
Friday:
Closed
Saturday:
Closed
Sunday:
Closed